How to Strengthen Your Lower Esophageal Sphincter (LES): A Registered Dietitian's Guide
If you've been told your lower esophageal sphincter is "weak" — and that there's not much you can do about it — I want you to hear this: your LES isn't broken. It's under-supported.
As a registered dietitian who specializes in acid reflux, GERD, and LPR, I've worked with hundreds of clients who were told some version of "you just have a weak sphincter." And almost every time, when we address the root contributors — diaphragmatic tone, nervous system regulation, intra-abdominal pressure, meal timing — their symptoms change. Sometimes dramatically.
That's because your LES — the lower esophageal sphincter, the small ring of muscle at the junction between your esophagus and stomach — doesn't function in isolation. It's part of an architecture. And when we support that architecture, LES pressure improves.
Let me walk you through exactly how.
What Your LES Actually Does (And Why It Matters)
Your LES is supposed to open when you swallow food and close tightly afterward to keep stomach acid where it belongs — in your stomach. When LES pressure is too low or the sphincter relaxes at the wrong time, acid moves upward into your esophagus. That's reflux.
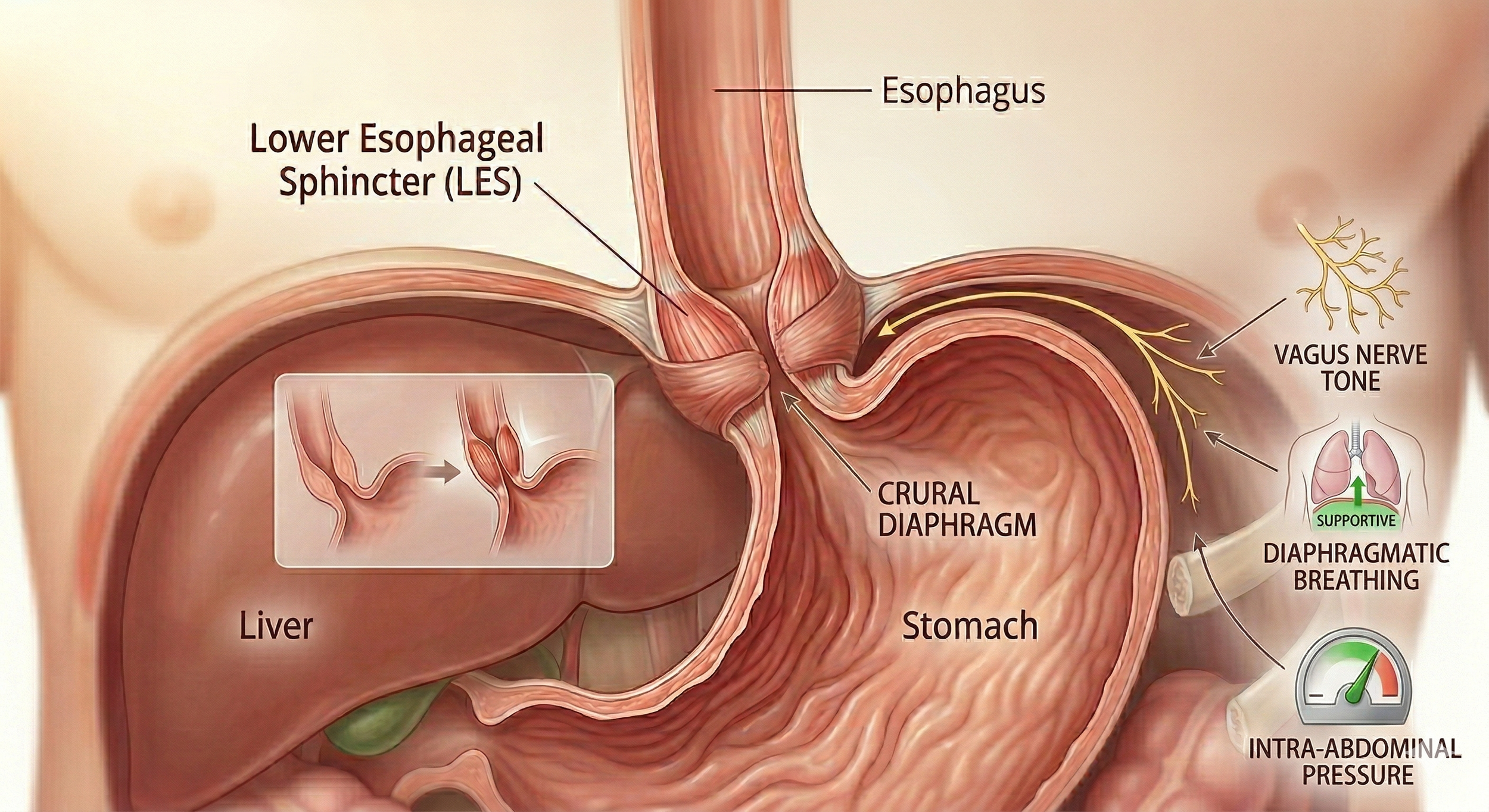
But here's what most people don't know: your LES doesn't work alone. It works in coordination with your crural diaphragm — the muscular portion of your diaphragm that wraps around the LES like a second sphincter. Together, they form what researchers call the "anti-reflux barrier."
When either component is under-supported — through chronic stress, shallow breathing, high intra-abdominal pressure, poor meal timing, or reduced vagal nerve tone — the whole system becomes less effective. The acid goes up. The symptoms follow.
This is barrier mechanics. And it's the foundation of how I approach reflux with every client.
6 Evidence-Based Ways to Strengthen Your LES
This is the single most underused intervention for acid reflux — and one of the most effective.
Your crural diaphragm wraps around your LES. When you practice slow, deep diaphragmatic breathing, you're actively strengthening that external support system. The research backs this up: a randomized controlled study by Eherer et al. (2012) in the American Journal of Gastroenterology (PMID: 22146488) found that patients who practiced diaphragmatic breathing exercises saw a significant decrease in esophageal acid exposure time — from 9.1% to 4.7% (p<0.05) — along with improved quality of life and reduced PPI usage.
A more recent RCT (Halland et al., 2021, PMID: 33009052) confirmed that diaphragmatic breathing increased LES pressure during the inspiratory phase from 23.1 mmHg to 42.2 mmHg and reduced postprandial reflux events from 2.60 to 0.36.
How to practice: Lie on your back with your knees bent. Place one hand on your chest and one on your belly. Breathe in slowly through your nose for 4 counts, feeling your belly rise while your chest stays still. Exhale slowly for 6 counts. Practice for 5–10 minutes, ideally 1 hour after meals, up to 5 times daily. Check out this blog: Diaphragmatic Breathing for Acid Reflux: How 10 Minutes a Day Can Strengthen Your LES
This is what I call "The LES Lock" — and it's one of the foundational tools in the FLORA method.
2. Meal Timing and the 4-Hour Buffer
Your LES is under the most pressure when your stomach is full. The more distended your stomach, the more likely transient LES relaxations will occur — and the more likely acid will escape upward.
This is why eating your last meal at least 3–4 hours before lying down makes such a measurable difference. When you lie down with a full stomach, you remove the protective effect of gravity and increase the pressure gradient across your LES.
What to do: Stop all food and drink (other than water and medications) at least 3 hours before bed. If your symptoms are significant, extend that to 4 hours. This single change reduces intragastric pressure during sleep and gives your LES the best chance of staying closed.
3. Left-Side Sleep Positioning
The anatomy of your stomach means that sleeping on your left side places your LES in a gravity-favorable position — essentially creating an "air pocket" above your stomach contents, so acid has to travel uphill to reach the sphincter.
Sleeping on the right side or flat on your back does the opposite: it positions the gastric pool directly adjacent to the LES, making reflux events more likely.
What to do: Sleep on your left side and elevate the head of your bed 6–9 inches using a wedge pillow or bed risers. This is not the same as stacking pillows under your head (which can actually increase abdominal pressure). The goal is a gentle incline from the waist up.
4. Reducing Intra-Abdominal Pressure
Anything that increases pressure in your abdominal cavity pushes upward against your stomach — and against your LES. This includes tight clothing, heavy lifting with poor breathing mechanics, excess visceral adiposity, and chronic straining during bowel movements.
What to do: Avoid tight waistbands and high-compression clothing around your midsection, especially after meals. If you strength train, coordinate your breathing — exhale on exertion rather than holding your breath (which spikes intra-abdominal pressure). If constipation is part of your picture, addressing motility is part of addressing reflux. They're connected.
5. Nervous System Regulation
This is the one most people miss — and it's one of the most important root contributors to reflux.
When your nervous system is in a stress-dominant state (sympathetic activation, or "fight or flight"), your body deprioritizes digestion. Blood flow shifts away from your gut. Your diaphragm tightens. Your LES coordination is disrupted. Gastric motility slows.
You can eat the exact same meal on two different days and have completely different reactions — simply because your stress levels were different. That's not in your head. That's physiology.
What to do: Practice the 5+1 Method before meals: 5 deep diaphragmatic breaths plus 1 moment of gratitude. This activates your parasympathetic nervous system — your "rest and digest" system — and primes your entire digestive tract for better coordination, including your LES.
6. Strategic Fiber Supplementation
Fiber — specifically soluble fiber like psyllium — supports LES function through multiple mechanisms. It help support healthy motility and bowel regularity, which prevents constipation and reduces excess pressure on the LES. It also creates a viscous texture in the stomach when combined with water and food contents, which is thicker and harder to reflux upwards into the esophagus. Lastly, it supports the microbiome, which may help to support digestion and reduce excess fermentation, which can put pressure on the LES.
A prospective randomized trial by Rana et al. (2025) in the Indian Journal of Otolaryngology and Head Neck Surgery (PMID: 40226240) studied 505 patients with confirmed LPR over 16 weeks and found that psyllium husk supplementation outperformed prokinetics across every outcome measure — including symptom scores, laryngeal findings, and quality of life.
What to do: Talk with your dietitian or healthcare provider about adding psyllium husk strategically — typically 5g mixed in water, taken with meals. The form, timing, and dose matter and may differ depending on the person and reflux type.
What This All Adds Up To
Your LES isn't a broken valve that needs surgery or lifelong medication to manage. In many cases, it's a muscle that's part of a larger system — and when you support that system with the right breathing practices, meal timing, sleep positioning, nervous system regulation, and strategic supplementation, LES pressure improves. Reflux events decrease. Symptoms change.
This is barrier optimization. Not symptom suppression.
And this is exactly the kind of multi-layered approach we map out inside the Reflux Relief Masterclass — my signature program where I walk you through the full FLORA method step by step: barrier mechanics, nervous system regulation, LES support, food strategy, and supplement protocols. If you've been doing "all the right things" and still struggling, this is where we go deeper.
→ Join the Reflux Relief Masterclass
You deserve support that actually explains why your body is doing what it's doing — and what to do about it. This is the work.
With love,
Molly Pelletier, MS, RD