How to Tell If Your Reflux Is Meal-Related or Stress-Related
You've been tracking your meals. You've cut out trigger foods. You eat early, you chew slowly, you sleep on a wedge pillow. And still—your reflux persists.
Here's what most people don't realize: Not all reflux is caused by food.
In fact, some of the most stubborn, treatment-resistant GERD cases have little to do with what you're eating—and everything to do with how your nervous system is functioning.
At FLORA, we treat reflux as a nervous system and pressure management issue, not just a dietary one. Understanding whether your reflux is meal-related, stress-related, or both is the first step toward real, lasting relief.
The Two Pathways of Reflux
Before we dive into how to differentiate between meal-related and stress-related reflux, let's clarify the mechanisms at play.
Meal-Related Reflux
This type of reflux is triggered by:
Specific foods that relax the lower esophageal sphincter (LES) or delay gastric emptying (e.g., caffeine, chocolate, high-fat meals, peppermint)
Large meal volume that increases intra-abdominal pressure
Timing issues like eating too close to bedtime or lying down after meals
Meal-related reflux typically follows a predictable pattern: you eat a trigger food or large portion, and within 30 minutes to 2 hours, you experience heartburn, regurgitation, or throat discomfort.
Stress-Related Reflux
This type of reflux is driven by:
Chronic stress or anxiety that activates the sympathetic nervous system
"fight or flight" response can lead to increased acid production as the body prepares for perceived threats
Poor vagal tone, which reduces LES pressure and slows gastric motility
Visceral hypersensitivity, where higher levels of stress can hypersensitize the esophageal tissue to have feelings of reflux even when it's not happening
Stress-related reflux often occurs even when you're eating "safe" foods. It's unpredictable, doesn't follow meal timing, and may worsen during periods of high stress, lack of sleep, or emotional distress.
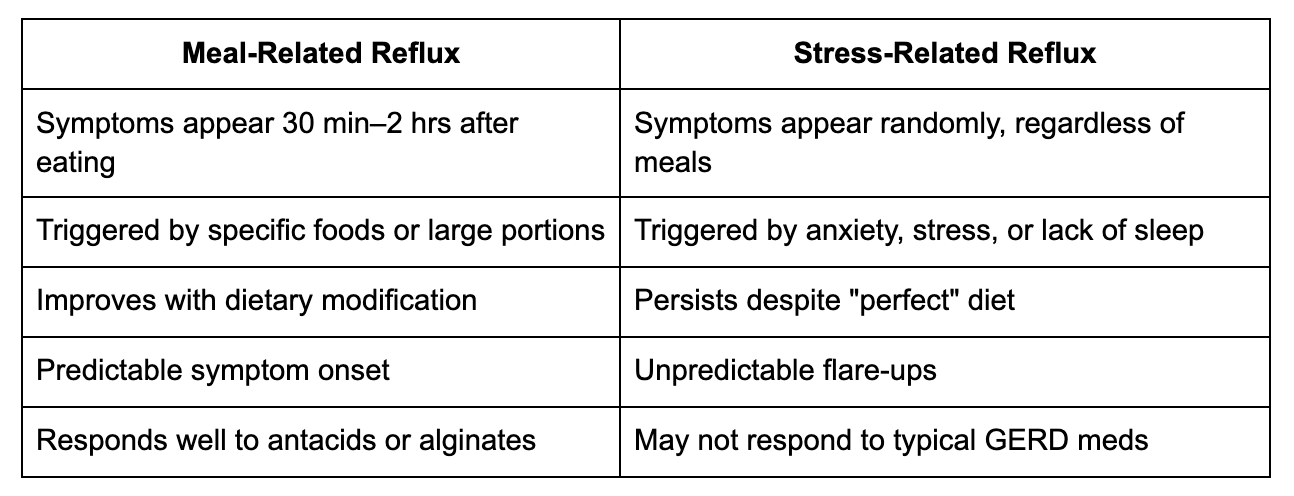
Key Differences: Meal-Related vs. Stress-Related Reflux
How to Identify Your Reflux Pattern
Here's a step-by-step framework to determine whether your reflux is meal-related, stress-related, or both.
Step 1: Track Symptoms + Context (Not Just Food)
Most people track what they eat. But to identify stress-related reflux, you need to track:
Time of day
Meal size and composition
Stress level (1–10 scale)
Sleep quality the night before
Life events (deadlines, arguments, travel, etc.)
Step 2: Look for Meal-Independent Flares
Ask yourself:
Do I get reflux on an empty stomach?
Do I wake up with reflux even though I finished eating 4+ hours before bed?
Do my symptoms worsen during stressful periods—even when my diet hasn't changed?
If you answered yes to any of these, stress is likely a major contributor.
Step 3: Test the Nervous System Hypothesis
Try this experiment:
For 3 days, practice 10 minutes of diaphragmatic breathing (details later in the blog) before each meal.
Eat the same meals you'd normally eat (no dietary changes).
Track your symptoms.
If your symptoms improve significantly without changing your diet, your reflux is at least partially stress-driven.
Step 4: Assess Your Vagal Tone
The vagus nerve regulates LES pressure, gastric motility, and the stress response. Low vagal tone is common in people with chronic stress and correlates with worse GERD symptoms.
Signs of low vagal tone:
Difficulty relaxing
Shallow breathing
Slow gastric emptying (early satiety, bloating)
Heart rate variability (HRV) below 50 (if you track this)
If you have multiple signs, stress-related reflux is highly likely.
What to Do If Your Reflux Is Meal-Related
If your reflux follows a clear meal-trigger pattern:
Use the 3-2-1 Rule
Optimize meal volume. Smaller, more frequent meals (ex. 3 meals) reduce intra-abdominal pressure. Some may have 4-5 meals; that is okay.
Time your meals strategically. Finish eating at least 2 hours before lying down.
Identify and rotate triggers. Don't eliminate forever. 1 trigger per day maximum.
What to Do If Your Reflux Is Stress-Related
If your reflux persists despite dietary changes, your nervous system needs support:
1. Diaphragmatic Breathing
Research shows diaphragmatic breathing as a successful intervention for stress-related reflux.1 It strengthens the crural diaphragm (which supports the LES), activates the vagus nerve, and reduces sympathetic tone.
How to do it:
Sit or stand tall.
Place one hand on your chest, one on your belly.
Notice without judgement what's moving when breathing
Inhale through your nose for 4 counts (belly expands, chest stays still).
Exhale through your mouth for 6 counts.
Repeat for 5–10 minutes, 1–2x per day.
Not only does it help relieve reflux but also decrease stress.
2. Sleep Optimization
Poor sleep worsens reflux. Prioritize 7–9 hours and elevate your head 6–8 inches.
4. Gut-Brain Axis Support
The gut and brain communicate bidirectionally via the vagus nerve. Supporting your microbiome with fruits and vegetables that contain soluble fiber, and prebiotic fibers can improve vagal tone and reduce reflux.
5. Create a Stress Management Routine
Start small
Schedule into your day and make this a non-negotiable
Utilize reminders and visual cues
Remember your why
Stay consistent - even if stress goes away
Journaling
What are your biggest sources of stress?
Are any of these sources of these stressors modifiable (boundaries)?
What helps you reduce stress?
Design
Highlight or circle the activities you are interested in or willing to explore
Meditation, or Gut-Directed Meditation on the FLORA App
Movement: walking, yoga, stretching, dancing
Self-Care: self-massage, essential oils, showers (hot or cold)
Joy Producing Hobbies: music, gardening, cooking
Connection: calling a friend or family member
Habit Stacking - can you stack your new mindfulness/stress management on top of a current habit
Most People Have Both
Here's the truth: most reflux patients have a combination of meal-related and stress-related triggers.
You might have certain foods that worsen symptoms, but stress amplifies their effect. Or you might eat perfectly and still flare during high-stress periods.
This is why the FLORA framework focuses on addressing diet, motility, pressure management, and nervous system regulation simultaneously.
The Bottom Line
Reflux isn't always about food. If you've been restricting your diet without results, it's time to look at your nervous system, stress levels, and vagal tone.
Understanding whether your reflux is meal-related, stress-related, or both allows you to target the right interventions and finally break the cycle.
Ready for a Personalized Approach?
To move beyond the cycle of constant flares and build a personalized nutrition roadmap that prioritizes long-term recovery, our FLORA 1:1 nutrition counseling program provides the expert, evidence-based guidance you need to heal with clarity. You can learn more and apply HERE.
For everyday support, including gut-soothing recipes and meditation and breathing exercises, the FLORA app serves as your digital companion for a life without the burn. By staying committed to these foundational shifts and utilizing the right tools, you can move forward with the comfort and peace of mind you deserve.
References:
Halland M, Bharucha AE, Crowell MD, Ravi K, Katzka DA. Effects of Diaphragmatic Breathing on the Pathophysiology and Treatment of Upright Gastroesophageal Reflux: A Randomized Controlled Trial. Am J Gastroenterol. 2021;116(1):86-94. doi:10.14309/ajg.0000000000000913
👩⚕️ Author:
Molly Pelletier, MS, RD, is a Registered Dietitian specializing in Gastroesophageal Reflux Disease (GERD), Laryngopharyngeal Reflux (LPR), and integrative gut health nutrition. Through FLORA, she helps clients resolve complex GI symptoms using evidence-based, root-cause protocols.