How to Stop GERD Naturally: The Ultimate Guide to Alginates and Mucilaginous Herbs
If you’ve been told that GERD is simply a “too much stomach acid” problem, you’ve been given an incomplete explanation. Acid reflux is rarely about excess acid, it’s about stomach contents moving in the wrong direction due to impaired digestion or motility issues.
Most conventional treatments focus on suppressing acid. Antacids neutralize it. H2 blockers reduce it. PPIs significantly shut it down. These approaches can help manage symptoms, but they don’t address an important part of the picture.
What about the tissue that acid already damaged?
Because when your esophageal lining is inflamed, thinned, and hypersensitive, even small amounts of reflux can feel unbearable. The key isn’t just stopping acid — it’s restoring esophageal mucosal integrity.
Today, we’re going beyond symptom suppression and talking about how to actually rebuild your mucosal barrier using alginates and mucilaginous herbs.
What’s Really Driving Persistent GERD Symptoms?
1. Esophageal Mucosal Integrity
Your esophagus is lined with epithelial cells protected by a thin mucosal barrier. This barrier acts like a biological shield, preventing acid and digestive enzymes from penetrating deeper tissue layers. When that barrier is compromised, inflammation increases and symptoms intensify.
2. Pepsin-Driven Inflammation
Pepsin is a digestive enzyme designed to break down protein in the stomach. When reflux occurs, pepsin can travel upward and embed itself into esophageal tissue. Even in low-acid environments, pepsin can reactivate and continue causing pepsin-driven inflammation. This means acid suppression alone doesn’t eliminate tissue irritation.
3. Visceral Hypersensitivity
Once tissue is inflamed, nerve endings become more reactive. This is called visceral hypersensitivity, and it explains why some people feel intense burning even when reflux volume is minimal.
When the lining is damaged, everything feels worse. Healing the tissue reduces that hypersensitivity.
The Mucosal Barrier: Your First Line of Defense
Think of your esophageal lining like protective paint on a wall.
If the paint is intact, the wall underneath is protected.
If the paint peels, even minor exposure causes damage.
The mucosal barrier is that protective coating.
Rebuilding it does three powerful things:
Shields tissue from acid and pepsin
Reduces inflammatory signaling
Calms nerve hypersensitivity
This is where alginates and mucilaginous botanicals shine.
Alginates
Most GERD treatments try to reduce acid production. Alginates take a completely different approach. Instead of changing how much acid your stomach makes, they physically block reflux from traveling upward in the first place.
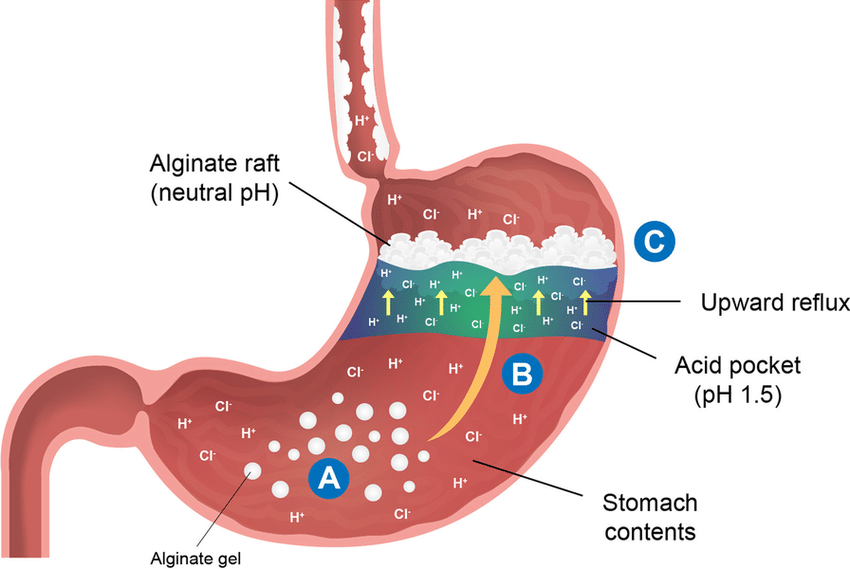
The “Acid Pocket” Problem
After you eat, acid doesn’t mix evenly with food right away. It forms what researchers call the postprandial acid pocket, a highly acidic layer that sits at the top of stomach contents near the lower esophageal sphincter.¹
This pocket is often the main source of reflux episodes. So even if overall acid production is normal, that concentrated acid layer can easily flow upward, especially if the sphincter is weak or relaxed.
Reflux Raft: A Mechanical Barrier That Makes Sens
Alginic acid derivatives (alginates) react with gastric acid to form a thick gel.
In the presence of stomach acid, they precipitate into a floating “raft” that localizes right over the acid pocket in the proximal stomach. Think of it like placing a protective lid over the most irritating part of your stomach contents. Instead of acid splashing upward, the alginate raft rises first creating a mechanical barrier.¹
This makes them ideal for:
Immediate symptom relief
Protecting the esophagus during healing
Supporting long-term mucosal repair
What the Research Shows
A large meta-analysis evaluated 14 randomized controlled trials studying alginate therapy for symptomatic GERD.¹ People taking alginates were more than four times as likely to experience meaningful symptom relief compared to placebo or antacids. That’s not just soothing. That’s clinically significant protection.
I consistently recommend Reflux Raft to my clients because of its unique alginate formula that has helped so many of them finally find relief from persistent symptoms. Shop Reflux Raft here.
Mucilaginous Herbs That Rebuild the Barrier
“Mucilaginous” means rich in plant compounds that form soothing, gel-like substances when mixed with water. These botanicals coat irritated tissue and support epithelial regeneration.
Let’s look at the research-backed standouts.
Slippery Elm
Slippery elm (Ulmus rubra) is made from the ground, dried inner bark of the tree and has a long history of use for inflammatory conditions involving mucous membranes, particularly in the gastrointestinal and upper airway tract.They are rich carbohydrates that swell when mixed with water to form a thick, gel-like substance. This mucilage coats irritated tissue, creating a soothing, protective layer that can help reduce discomfort, inflammation, and reflexive responses like coughing or throat clearing.²
DGL (Deglycyrrhizinated Licorice)
DGL stimulates mucus production and supports mucosal blood flow, which enhances healing.³ Unlike whole licorice, DGL removes glycyrrhizin, the compound that can raise blood pressure, making it safer for longer-term use.
L-Glutamine
Glutamine is the most abundant amino acid in the body and a key fuel source for intestinal epithelial cells. While mucilaginous herbs coat irritated tissue, glutamine helps rebuild it from the inside out.⁴ L-Glutamine is the primary fuel source for intestinal epithelial cells. In the small intestine, it supports:
Cell proliferation and regeneration
Repair of damaged mucosal tissue
Maintenance of tight junctions (the “seals” between gut cells)
Prevention of excess intestinal permeability
Evidence shows that glutamine helps preserve gut barrier function and reduces permeability to toxins and pathogens, especially during periods of gastrointestinal stress or injury.⁴ In fact, during periods of physical stress, illness, or intense exercise, when glutamine demands increase and levels may drop, adequate glutamine becomes essential for protecting the mucosa and preventing increased intestinal permeability that can drive inflammation and irritation.
Zinc Carnosine
If there were a single compound designed specifically to heal damaged GI tissue, it would look a lot like zinc carnosine. Zinc carnosine has been studied extensively for gastric mucosal healing. It protects cells, reduces inflammatory signaling, and helps stabilize damaged tissue so it can regenerate.⁵ And importantly, it works locally and directly on damaged mucosa, which is exactly what we want when addressing esophageal and gastric inflammation.
If paired with alginates, it forms a protective raft that blocks acid and helps zinc L-carnosine stay in contact with irritated tissue longer. Together, they protect the lining while giving it a better chance to repair and heal.
This is exactly why I developed Sequoia Soothe. I wanted to create a comprehensive formula that not only provides relief, but also the building blocks to actually repair the esophageal lining. Containing miscellaneous herbs like DGL, Slippery Elm, L-Glutamine and Zinc Carnosine, it’s the all-in-one approach my clients have used to move past the “band-aid” phase.
Final Thoughts
GERD isn’t just about acid. It’s about barrier integrity. When you shift from “How do I stop acid?” to “How do I heal tissue?” Everything changes.
Remember:
Protect with alginates.
Rebuild with mucilaginous herbs.
Restore your mucosal barrier.
Move beyond the band-aid.
Ready to protect and rebuild your esophageal lining?
Explore Sequoia Soothe HERE.
References:
Leiman DA, Riff BP, Morgan S, et al. Alginate therapy is effective treatment for GERD symptoms: a systematic review and meta-analysis. Dis Esophagus. 2017;30(5):1-9. doi:10.1093/dote/dow020
Watts CR, Rousseau B. Slippery elm, its biochemistry, and use as a complementary and alternative treatment for laryngeal irritation. Journal of Investigational Biochemistry. 2012; 1(1):17-23. doi:10.5455/jib.20120417052415
Ghalayani P, Emami H, Pakravan F, et al. Comparison of triamcinolone acetonide mucoadhesive film with licorice mucoadhesive film on radiotherapy-induced oral mucositis: A randomized double-blinded clinical trial. Asia-Pacific Journal of Clinical Oncology. 2014;13(2):48-56. doi: 10.1111/ajco.12295
Rao R, Samak G. Role of Glutamine in Protection of Intestinal Epithelial Tight Junctions. J Epithel Biol Pharmacol. 2012;5(Suppl 1-M7):47-54. doi:10.2174/1875044301205010047
Efthymakis K, Neri M. The role of Zinc L-Carnosine in the prevention and treatment of gastrointestinal mucosal disease in humans: a review. Clin Res Hepatol Gastroenterol. 2022;46(7):101954. doi:10.1016/j.clinre.2022.101954
👩⚕️ Author:
Molly Pelletier, MS, RD, is a Registered Dietitian specializing in Gastroesophageal Reflux Disease (GERD), Laryngopharyngeal Reflux (LPR), and integrative gut health nutrition. Through FLORA, she helps clients resolve complex GI symptoms using evidence-based, root-cause protocols.
Healing from chronic reflux requires more than just avoiding "trigger foods"—it requires a strategic plan to restore your gut’s natural defenses. To move beyond the cycle of constant flares and build a personalized nutrition roadmap that prioritizes your tissue repair and long-term recovery, our FLORA 1:1 nutrition counseling program provides the expert, evidence-based guidance you need to heal with clarity. You can learn more and apply HERE.
For everyday support, including gut-soothing recipes and targeted protocols for mucosal health, the FLORA app serves as your digital companion for a life without the burn. By staying committed to these foundational shifts and utilizing the right tools, you can move forward with the comfort and peace of mind you deserve.