Low FODMAP 101: How to Calm IBS and Acid Reflux Without Restricting Foods for Life
When Your Gut Feels Out of Control
If your gut has ever felt completely out of control, you’re not alone. Bloating, gas, stomach pain, and unpredictable digestion can make everyday life uncomfortable—and sometimes even stressful. For many, these symptoms appear without warning, making it impossible to know which foods help or hurt
Something many people don’t realize is that digestive conditions often overlap. Individuals who struggle with acid reflux (GERD or LPR) also frequently experience symptoms of Irritable Bowel Syndrome (IBS) [1].
The good news? One of the most researched approaches for managing IBS and overlapping digestive discomfort is the Low FODMAP diet. This strategy helps you identify specific triggers so you can stop guessing and start feeling better.
Crucial Note: The Low FODMAP diet is not a "forever" diet. It is a temporary, short-term strategy to help you return to a flexible, balanced way of eating.
What are the Symptoms of IBS?
Irritable Bowel Syndrome (IBS) is a common digestive condition affecting up to 5-10% of people worldwide [2]. It is characterized by recurrent abdominal pain and changes in bowel habits, such as diarrhea, constipation, or a mix of both.
Common symptoms include:
Bloating and Gas: Feeling excessive pressure or "fullness" in the abdomen.
Abdominal Pain: Cramping that often fluctuates in intensity.
Unpredictable Digestion: Flares that come and go based on stress or diet.
As a digestive health dietitian, I remind my clients that IBS management isn't one-size-fits-all. Because triggers vary—some react to food, others to stress—understanding your unique gut sensitivity is the first step toward long-term relief.
What Does FODMAP Stand For?
The Low FODMAP diet reduces a specific group of short-chain carbohydrates that are often poorly absorbed in the small intestine. When these carbs aren't digested properly, they ferment in the gut, leading to the gas and bloating typical of IBS and GERD.
FODMAP is an acronym for:
Fermentable
Oligosaccharides (e.g., wheat, onions, garlic)
Disaccharides (e.g., lactose in dairy)
Monosaccharides (e.g., excess fructose in honey or apples)
Polyols (e.g., sorbitol and mannitol in certain fruits and sweeteners)
By removing these for a short window, you give your digestive system a chance to "reset."
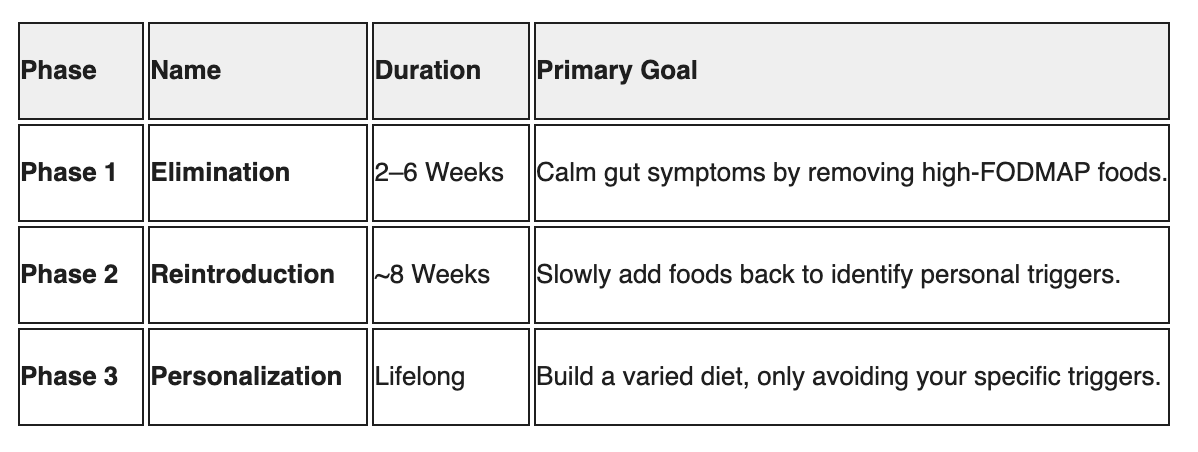
The 3 Phases of the Low FODMAP Diet
To find relief without lifelong restriction, we follow a structured three-phase process:
The ultimate goal of Phase 3 is to expand your diet, not keep it restricted [3].
High-FODMAP vs. Low-FODMAP Food List
It’s important to remember that high-FODMAP foods aren't "bad"—many are highly nutritious. We simply limit them temporarily to find your threshold.
Common Foods to Swap
Instead of Garlic & Onions: Try chives, the green tops of spring onions, or garlic-infused oil.
Instead of Apples & Pears: Try strawberries, grapes, or kiwi.
Instead of Wheat Bread: Try sourdough (spelt or white) or certified gluten-free options.
Instead of Beans/Legumes: Try firm tofu or small servings of canned lentils (rinsed).
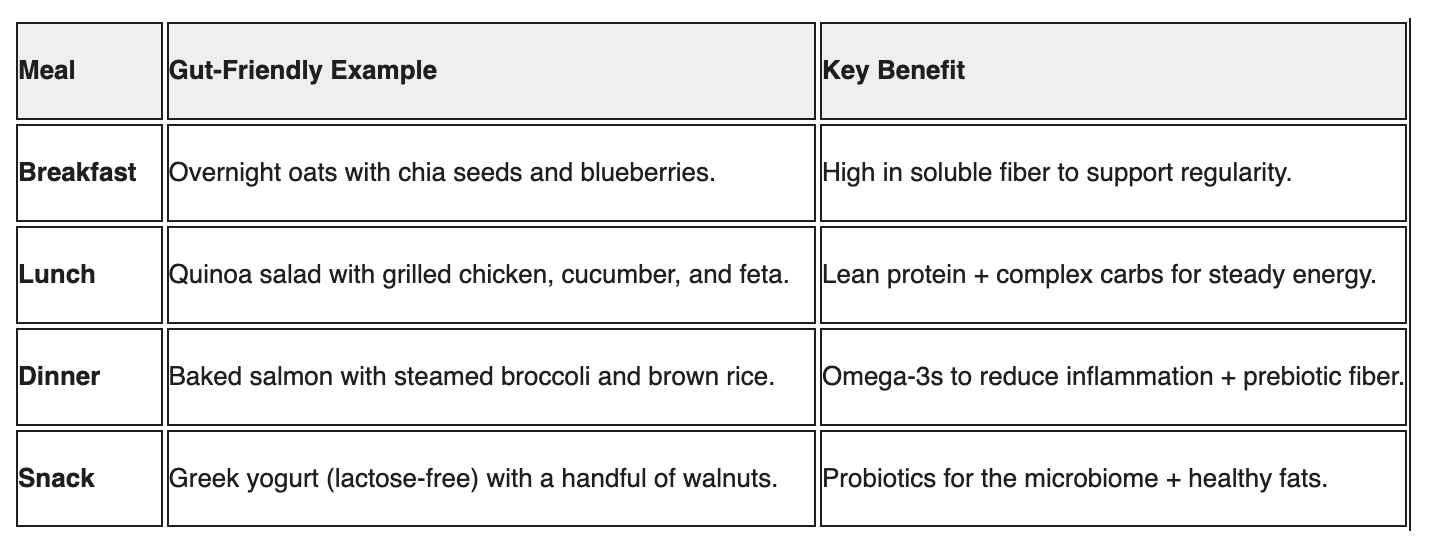
A Sample Day of Low-FODMAP Eating
Why You Shouldn't Stay on Low FODMAP Forever
Staying on a restrictive version of this diet long-term can actually backfire.
Gut Health: Many high-FODMAP foods act as prebiotics that feed beneficial gut bacteria.
Nutrient Variety: Long-term restriction limits the diverse vitamins and minerals your body needs.
Mental Health: Eating should be enjoyable! Restricting foods indefinitely can lead to unnecessary stress and "food fear."
Tips for Success: Eating Out and Starting Out
If you are ready to start, keep these practical tips in mind:
Work with a Dietitian: A professional ensures you stay nutritionally balanced during elimination.
Plan Ahead: Check restaurant menus online for "plain" protein options like grilled fish or steak.
Ask for Modifications: Request that sauces or dressings be served on the side, as these often contain hidden garlic and onion.
Portion Sizes Matter: Some foods are low FODMAP in small amounts but become high FODMAP in larger servings.
The Takeaway
IBS and acid reflux symptoms are frustrating, but they don't have to control your life. The Low FODMAP diet is a powerful, short-term tool to help you understand your body.
Ready to find relief?
You don’t have to figure this out alone. You can explore additional resources, including acid reflux and IBS-friendly recipes, inside the FLORA app. There, you’ll find tools like our "30 IBS-friendly snack ideas" guide.
If you’re ready to stop the guesswork and start a personalized plan, apply for a Roadmap Session today. Working with a dietitian one-on-one is the fastest way to identify your triggers and get back to eating the foods you love.
References
Alshammari SA, et al. Overlap Between Gastroesophageal Reflux Disease and Irritable Bowel Syndrome. Cureus. 2023.
About IBS: What is IBS? International Foundation for Gastrointestinal Disorders. 2023.
Low FODMAP Diet: What It Is & How to Follow. Cleveland Clinic. 2026.
👩⚕️ Author:
Molly Pelletier, MS, RD, is a Registered Dietitian specializing in Gastroesophageal Reflux Disease (GERD), Laryngopharyngeal Reflux (LPR), and integrative gut health nutrition. Through FLORA, she helps clients resolve complex GI symptoms using evidence-based, root-cause protocols.
Healing from chronic reflux requires more than just avoiding "trigger foods"—it requires a strategic plan to restore your gut’s natural defenses. To move beyond the cycle of constant flares and build a personalized nutrition roadmap that prioritizes your tissue repair and long-term recovery, our FLORA 1:1 nutrition counseling program provides the expert, evidence-based guidance you need to heal with clarity. You can learn more and apply HERE.
For everyday support, including gut-soothing recipes and targeted protocols for mucosal health, the FLORA app serves as your digital companion for a life without the burn. By staying committed to these foundational shifts and utilizing the right tools, you can move forward with the comfort and peace of mind you deserve.